At CardioVascular Health Clinic, your vascular and cardiovascular health means everything to us.
When you’re dealing with a vein-related condition such as pelvic congestion syndrome, we want to help.
Pelvic congestion syndrome affects approximately 15 to 40% of women aged 20 to 50. This condition causes chronic pelvic pain due to varicose veins within the pelvis.
If you or a loved one has been diagnosed with pelvic congestion syndrome or is at risk of developing the condition, it is vital to get evaluated and understand the treatment options available.
Let’s discuss pelvic congestion syndrome in more detail, including what it is, common symptoms, and innovative pelvic congestion syndrome treatment options.
Pelvic congestion syndrome, or pelvic venous insufficiency, is a vascular condition that causes blood to pool within varicose or bulging pelvis veins, leading to pain.
These abnormal veins can be secondary to abnormalities of the gonadal veins or compression of a vein in the pelvis called, May-Thurner. Unfortunately, this is a common yet underdiagnosed condition for many women with chronic pelvic pain.
Chronic pelvic pain is classified as pain in the lower abdomen or pelvis for over 6 months. Unfortunately, 60% of women with pelvic pain never get a proper diagnosis. The diagnosis for PCS is often not thought of during evaluation and workup.
People living with pelvic congestion syndrome often experience a number of symptoms ranging from mild to severe.
The most common symptoms include
While anyone, at any age, can develop pelvic congestion syndrome, you are considered at increased risk of developing this condition if you’ve had or currently have the following:
There are two main ways that we effectively treat pelvic congestion syndrome.
They include:
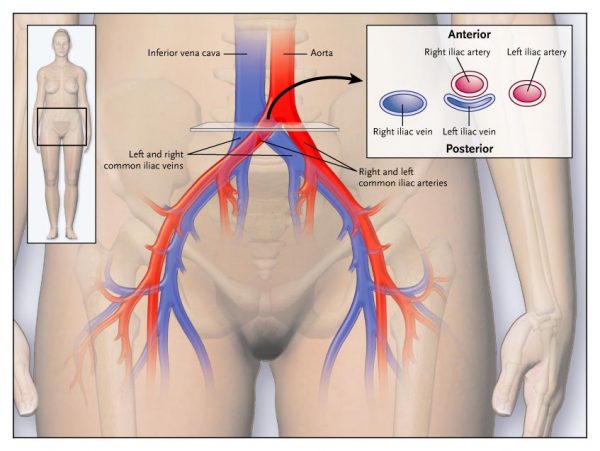
Iliac Venous Stenting
Pelvic congestion syndrome can be secondary to compression of the left common iliac vein, the draining vein in the pelvis. This is due to an anatomical compression of the right iliac artery compressing the left common iliac vein. By limiting blood drainage out of the pelvis, blood finds alternative routes through veins in the pelvis and spine, causing them to dilate and potentially cause pain.
This treatment option involves placing a stent within the compressed iliac vein to regain its standard size and decompressing venous pressure in the pelvis.
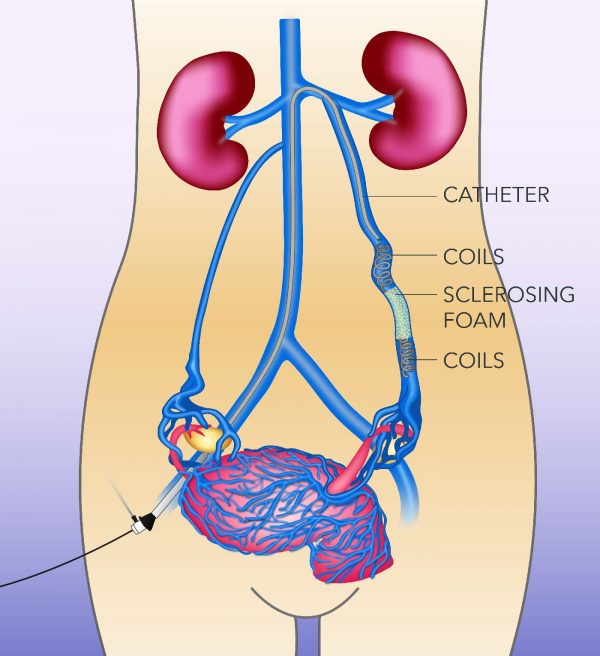
Ovarian Vein Embolization
Dilation of pelvic veins may be secondary to a leaky gonadal vein, allowing blood to back up into the pelvis instead of moving forward to the heart. This is diagnosed by performing a venogram or dye test with an X-ray to watch blood flow within the gonadal vein.
If reflux is noted, along with dilated varicose veins within the pelvis, this type of treatment is performed to shut down the vein with coils or embolized.
You shouldn’t have to live with chronic pelvic pain. You also shouldn’t have to manage your pain without a proper diagnosis.
The physicians at CardioVascular Health Clinic are qualified to diagnose and treat pelvic congestion syndrome and its potential life-altering symptoms.
If you or a loved one are experiencing symptoms consistent with pelvic congestion syndrome, we can help. We offer effective treatment options, like ovarian vein embolization, to help you eliminate pelvic pain and feel your best again.
Call us at 405-701-9880 or book a consultation online today.